restoreTAP Flap
Consultation RequestProcedure
The TAP Flap, or thoracodorsal artery perforator flap, is a small flap that utilizes tissue located on the side side of the breast, extending to the back, to reconstruct the breast. The TAP flap is located in the same region of the body as the latissimus flap. These flaps are similar in that the donor tissue used to reconstruct the breast is rotated from the upper back to the chest.
The TAP flap can be rotated from the upper back and positioned on the chest wall to use in partial breast reconstruction or to help correct a lumpectomy “dent”. The TAP flap contains skin and subcutaneous fat that lies over the latissimus dorsi muscle, but includes a perforating vessel that is attached to the thoracodorsal artery. Unlike the latissimus dorsi myocutaneous flap, the TAP flap preserves the back muscle. The TAP flap is what’s known as a ‘perforator flap’, meaning only skin and fat are harvested for the procedure and the muscle is left intact. Tiny blood vessels are carefully isolated and dissected from the muscle preserving the latissimus muscle, as well as the blood supply. With a latissimus flap, part of the back muscle is used for reconstruction, which can potentially limit movement in activities that require pushing off with the arm such as climbing or swimming.
The surgical time investment is greater with the TAP flap when compared to more traditional flap reconstruction procedures that sacrifice muscle. However, the benefits of preserving the muscle are often worth it, especially for active, athletic women. The resulting scar from TAP flap surgery can usually be placed horizontally and is well hidden in the bra strap line.
This is a small flap and most patients do not have enough tissue on the upper back to use TAP flaps alone in breast reconstruction after a mastectomy. The TAP flap is best used for small defects resulting after a lumpectomy, or as a combination procedure with implant placement and/or fat grafting to enhance the shape and size of the breast.
Candidates
You may be a candidate if:
- You have undergone or are planning to undergo a lumpectomy.
- You have breast deformity or skin deficit present due to prior breast surgery or radiation therapy.
- You have a small deficit present to the breast that does not require a large flap reconstruction and preserving your full latissimus muscle function is important to your active lifestyle.
Things to Consider:
- This is a more technical, and therefore, a lengthier procedure than latissimus flap breast reconstruction. This will result in a longer surgery and a hospital stay of 2 – 3 days.
- You will need support at home to help during your recovery process.
- Skin and fat located on the back is typically firmer than the tissue that makes up the breast or other areas of the body, such as the abdomen. This may result in a tighter feeling breast, as compared to other types of reconstruction.
- This is a two-stage procedure with the second stage of the procedure occurring no earlier than 3 – 4 months after the first stage.
- The first stage of the procedure focuses on safely transferring the tissue from the back to the breast.
- The second stage of the procedure focuses on refining the breast shape and volume and addresses symmetry between the breasts.
Benefits
Benefits of TAP Flap Reconstruction include:
- Full preservation of underlying latissimus dorsi muscle and shoulder function.
- Donor site scar on the back is easily concealed in the bra line.
- Improved contour and shape to the breast
Risks
The risks of flap breast reconstruction procedures are mainly related to the possibility of flap loss, but the TAP flap is kept on its original blood supply and is close in proximity to the chest, which minimizes this risk.
Recovery
Patients have a relatively short hospital stay of 2 – 3 days and can return to normal daily activities at approximately four weeks. You will be able to sleep on your back immediately after surgery. Most patients can resume all activities without restrictions, including lifting at 2 – 3 months.
As with any surgery, some swelling, bruising, and soreness are to be expected at first. You will be administered pain medication to help control any post-op discomfort. This tenderness and swelling should begin to subside after a few days. The majority of swelling should begin to resolve after a few weeks.
Results
You will have good short and long term results after TAP flap reconstruction. The tissue transferred during this reconstruction improves the contour and shape of the breast by replacing tissue removed or damaged during breast surgery or radiation therapy. It is important to note that back fat and skin is firmer compared to breast skin and fat. Therefore, the reconstructed breast will be affected less by changes in gravity than your natural breast.
Before & After Images
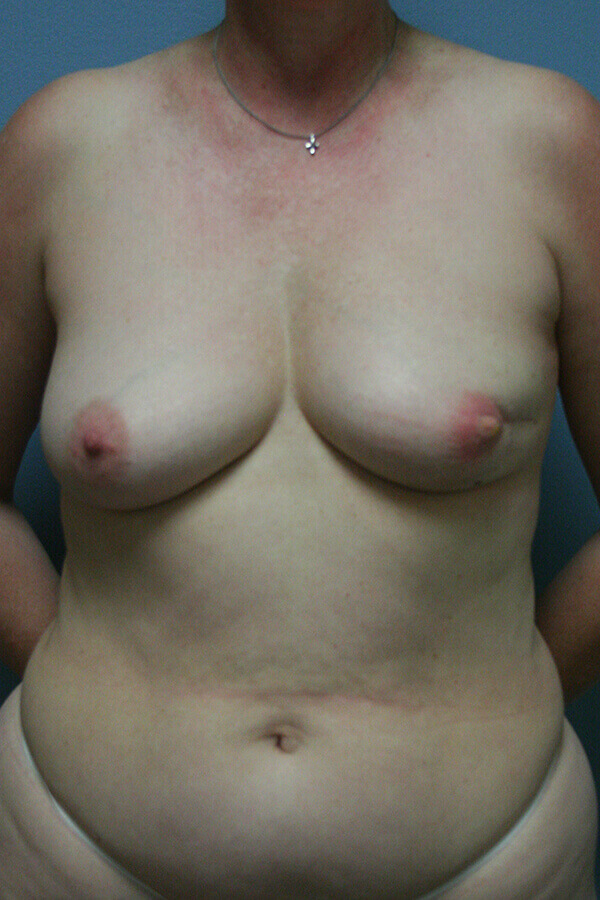
Before
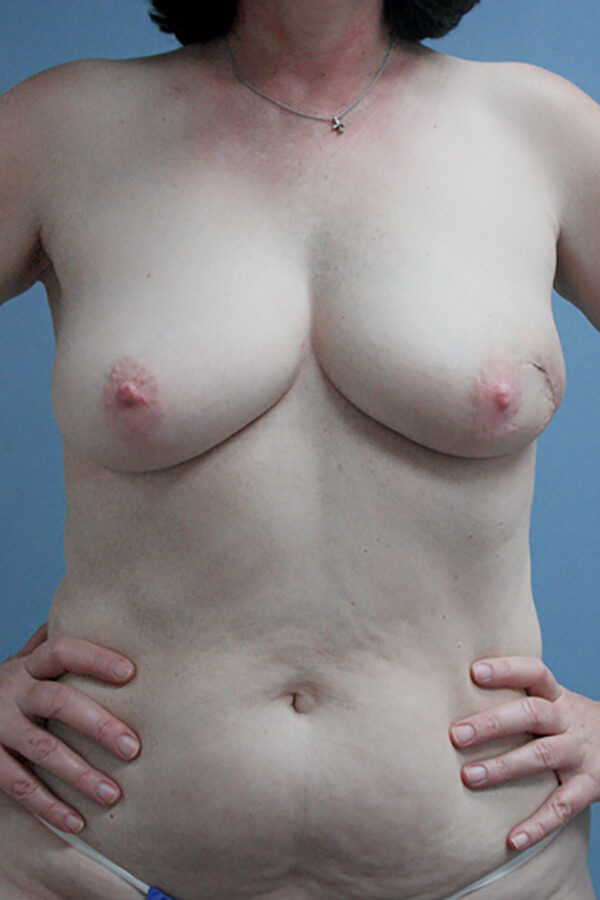
After
